How to Plan for Old Age Care
4. Make a plan for Pain Management for old age rehabilitation
Designing a pain management plan for old age rehabilitation involves addressing and alleviating pain, improving functional abilities, and enhancing the overall quality of life. Here’s a general outline to help you create a plan:
- Assess pain levels and causes: Begin by assessing the individual’s pain levels, location, and potential underlying causes. Consult with healthcare professionals, such as physicians or physiotherapists, to determine the nature of the pain and its potential sources, such as arthritis, neuropathy, or musculoskeletal conditions.
- Establish pain management goals: Collaborate with the individual and their healthcare team to establish realistic and specific pain management goals. These goals should focus on reducing pain intensity, improving functionality, and enhancing quality of life. It’s important to set goals that align with the individual’s abilities and preferences
- Medication management: Work with a healthcare professional to develop an appropriate medication management plan. This may involve prescribing pain relievers, anti-inflammatory medications, or other medications specifically targeted for the individual’s pain condition. Ensure that medications are taken as prescribed and monitor for any potential side effects or interactions.
- Physical therapy and exercise: Incorporate physical therapy and exercise into the pain management plan. A physical therapist can design a tailored exercise program that includes stretching, strengthening, and low-impact exercises to improve mobility, flexibility, and muscle strength. Regular exercise can help manage pain, increase blood flow, and release endorphins that act as natural pain relievers.
- Heat and cold therapy: Utilize heat and cold therapy as adjuncts to pain management. Heat therapy, such as warm showers, heating pads, or warm compresses, can help relax muscles and alleviate pain. Cold therapy, such as ice packs or cold compresses, can reduce inflammation and numb pain. Use these therapies based on the individual’s preferences and the recommendations of healthcare professionals.
- Assistive devices and adaptations: Identify and recommend assistive devices or adaptations that can help reduce pain and enhance functionality. This can include using walking aids, ergonomic chairs, supportive pillows, or adaptive equipment for activities of daily living. Properly fitting and using assistive devices can reduce strain on the body and minimize pain.
- Relaxation techniques: Introduce relaxation techniques to help manage pain and promote overall well-being. This can include deep breathing exercises, progressive muscle relaxation, guided imagery, or mindfulness meditation. These techniques can help reduce stress, enhance relaxation, and provide relief from pain.
- Complementary therapies: Explore complementary therapies that may assist in pain management. These may include acupuncture, massage therapy, chiropractic care, or alternative therapies like herbal remedies or aromatherapy. Consult with healthcare professionals experienced in these modalities to determine their suitability and effectiveness for the individual’s specific pain condition.
- Psychological support: Provide access to psychological support, such as counseling or therapy, to address the emotional impact of chronic pain. Chronic pain can lead to feelings of frustration, anxiety, or depression. Mental health professionals can help individuals develop coping strategies, manage emotional distress, and improve overall well-being.
- Regular evaluations and adjustments: Regularly assess the effectiveness of the pain management plan and make necessary adjustments. Monitor pain levels, functional improvements, and the individual’s overall satisfaction with the plan. Collaborate with healthcare professionals to ensure the plan is optimized and modified as needed.
Remember, pain management plans should be personalized to the individual’s specific needs and conditions. Consult with healthcare professionals, such as physicians, physiotherapists, or pain specialists, for personalized recommendations and guidance throughout the rehabilitation process.
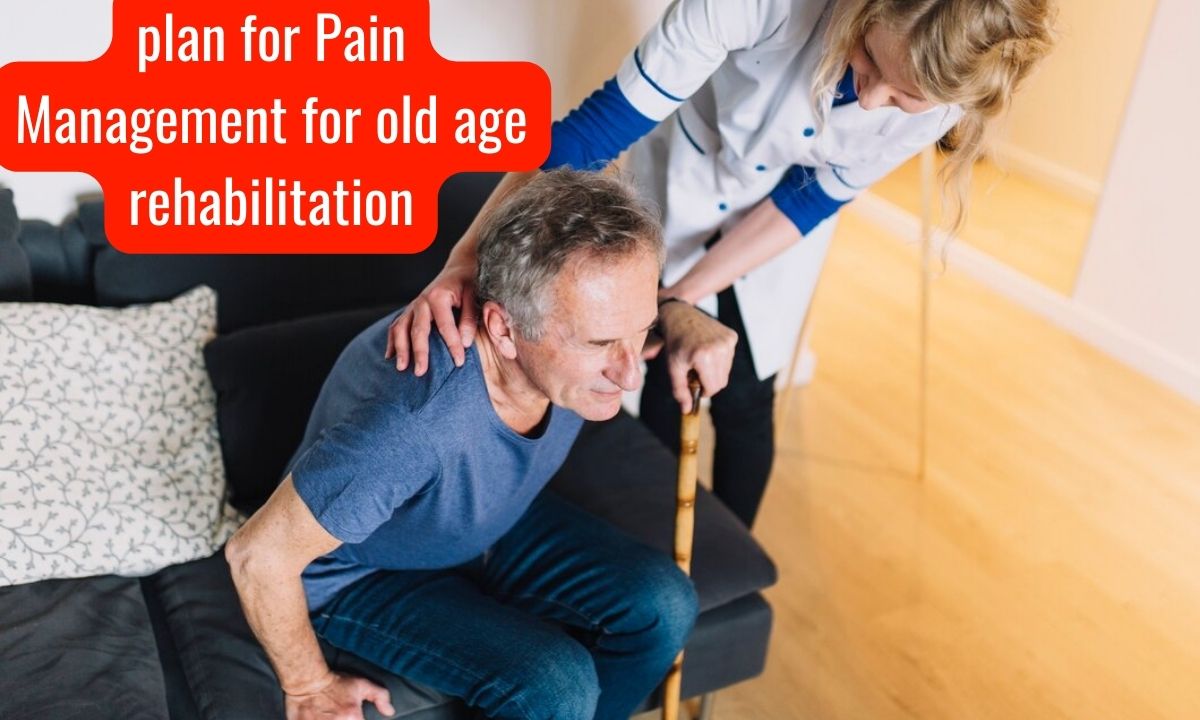
4.1 Support Factors in Pain Management for Rehab
Pain management is an essential component of rehab programs, especially for individuals recovering from injuries, surgeries, or chronic conditions. Here are some approaches and techniques commonly used for pain management in a rehabilitation setting:
- Medication Management: Depending on the type and severity of pain, healthcare professionals may prescribe medications such as nonsteroidal anti-inflammatory drugs (NSAIDs), opioids, muscle relaxants, or neuropathic pain medications. These medications should be carefully monitored and adjusted to ensure optimal pain relief while minimizing the risk of dependence or side effects.
- Physical Therapy: Physical therapists play a crucial role in pain management during rehab. They use various techniques such as therapeutic exercises, manual therapy, joint mobilization, and modalities like heat, cold, or electrical stimulation to alleviate pain, improve range of motion, and enhance functional abilities.
- Occupational Therapy: Occupational therapists help individuals manage pain and regain independence in daily activities. They may recommend adaptive equipment, and ergonomic modifications, and teach energy conservation techniques to minimize pain and maximize function.
- Psychological Interventions: Pain often has a psychological component, and addressing these factors can be beneficial in rehab. Cognitive-behavioral therapy (CBT), mindfulness-based stress reduction (MBSR), relaxation techniques, and biofeedback are commonly used to help individuals develop coping skills, modify thoughts and behaviors related to pain, and reduce psychological distress.
- Alternative and Complementary Therapies: Rehab programs may offer alternative or complementary therapies to manage pain. These may include acupuncture, massage therapy, chiropractic care, yoga, tai chi, or meditation. These approaches can promote relaxation, reduce muscle tension, improve circulation, and provide pain reliefEducation and Self-Management: Providing education about pain, its causes, and management strategies empower individuals to actively participate in their recovery. Rehab programs often teach self-management techniques such as pacing activities, proper body mechanics, stress reduction, and lifestyle modifications to minimize pain and optimize function.
- Assistive Devices and Orthotics: Depending on the nature of the pain and the specific needs of the individual, healthcare professionals may recommend the use of assistive devices such as canes, crutches, or orthotics. These devices provide support, improve mobility, and alleviate pain during rehab and daily activities.
- Multidisciplinary Approach: Pain management often requires a collaborative effort involving a multidisciplinary team of healthcare professionals. This team may include physicians, nurses, physical therapists, occupational therapists, psychologists, pain specialists, and social workers. They work together to develop an individualized pain management plan that addresses the unique needs and goals of the individual.
- Exercise and Conditioning: Engaging in appropriate exercise and conditioning programs can help manage pain, improve strength, flexibility, and endurance, and enhance overall function. Rehab programs often design tailored exercise regimens to gradually increase activity levels and reduce pain symptoms.
- Lifestyle Modifications: Encouraging healthy lifestyle habits can support pain management during rehab. This may involve promoting adequate sleep, a balanced diet, stress reduction techniques, weight management, smoking cessation, and avoiding activities or triggers that exacerbate pain.
It’s important for healthcare professionals to regularly assess and reassess pain levels, and treatment effectiveness, and adjust the pain management plan accordingly. Individualized care and ongoing communication between the patient and the rehab team are crucial for optimal pain management and successful rehabilitation outcomes.
5. Make a plan for Social Engagement for old age rehabilitation

Creating a plan for social engagement in old age rehabilitation involves promoting social connections, reducing isolation, and fostering a sense of community and belonging. Here’s a general outline to help you create a plan:
- Assess social needs and preferences: Begin by assessing the individual’s social needs, interests, and preferences. Understand their current social network, any challenges they may face in terms of isolation or limited social interactions, and their desired level of engagement. This assessment can be done through conversations, questionnaires, or by working with a social worker or geriatric care specialist.
- Identify opportunities for social engagement: Explore various opportunities for social engagement that align with the individual’s interests and abilities. This can include joining social clubs or organizations, attending community events, participating in group activities at community centers or senior centers, or becoming involved in volunteer work. Consider their hobbies, cultural background, and personal preferences when identifying suitable options.
- Encourage participation in group activities: Promote participation in group activities that foster social interaction and a sense of belonging. These activities can include exercise classes, art or craft groups, book clubs, game nights, or organized outings. Encourage the individual to actively engage in conversations, share experiences, and establish connections with others.
- Facilitate intergenerational interactions: Provide opportunities for intergenerational interactions, as they can be beneficial for both older adults and younger individuals. Encourage the individual to spend time with grandchildren, participate in mentoring programs, or volunteer in schools or youth organizations. Intergenerational interactions promote mutual learning, understanding, and a sense of purpose.
- Utilize technology for social connection: Incorporate technology as a means of social connection, especially for those who may have limited mobility or face geographic barriers. Encourage the use of social media platforms, video calls, or messaging apps to stay connected with family and friends. Provide guidance and support to help the individual navigate and utilize technology effectively.
- Establish support groups: Create or connect the individual with support groups or peer networks that focus on shared interests, life experiences, or specific health conditions. Support groups provide a platform for individuals to share their challenges, exchange advice, and receive emotional support from others who can relate to their experiences.
- Foster community involvement: Encourage community involvement and participation in local events and initiatives. This can include attending town hall meetings, participating in community service projects, or joining community committees or organizations. Engaging with the community promotes a sense of belonging and can lead to new friendships and social connections.
- Organize social outings: Plan and organize social outings or gatherings for the individual and their peers. This can involve outings to local attractions, cultural events, group meals, or day trips. Coordinate with community centers, senior centers, or local organizations to access resources and support for organizing such outings.
- Provide transportation assistance: Address transportation challenges that may hinder social engagement. Identify transportation options or resources available in the community, such as senior transportation services, volunteer driver programs, or accessible public transportation. Ensure the individual has access to reliable transportation to facilitate their participation in social activities.
- Regular evaluations and adjustments: Regularly evaluate the effectiveness of the social engagement plan and make necessary adjustments. Monitor the individual’s social connections, participation, and overall satisfaction. Seek feedback from the individual and their support network to identify areas of improvement and implement necessary changes.
Remember, social engagement plans should be tailored to the individual’s needs, preferences, and abilities. Collaborate with social workers, geriatric care specialists, or community organizations to access additional resources, support, and guidance throughout the rehabilitation process.
5.1 Support Factors in the Social Engagement for Rehab
Social engagement plays a significant role in the rehabilitation process as it promotes connection, support, and a sense of belonging. Here are some important aspects of social engagement that can be incorporated into rehab programs:
- Group Therapy: Group therapy sessions provide a structured and supportive environment for individuals in rehab to share their experiences, challenges, and successes with others who are going through similar journeys. These sessions foster a sense of community, empathy, and mutual support, promoting social engagement.
- Support Groups: Support groups, whether facilitated by professionals or peer-led, allow individuals to connect with others facing similar challenges. These groups provide a platform for sharing experiences, offering advice, and receiving emotional support. Support groups can be focused on specific conditions (e.g., addiction, chronic pain) or broader topics related to rehabilitation.
- Family Involvement: Encouraging family involvement in rehab can enhance social engagement and strengthen support networks. Involving family members in therapy sessions, educational programs, and family counseling can promote understanding, communication, and positive relationships, which are crucial for long-term recovery.
- Community Integration: Engaging individuals in rehab with their local community can foster a sense of belonging and provide opportunities for social interaction. This can be done through organized outings, community events, volunteer work, or involvement in local support groups or organizations related to their recovery or interests.
- Recreational Activities: Incorporating recreational activities into rehab programs promotes social engagement and provides opportunities for individuals to develop new hobbies, interests, and social connections. Activities such as sports, art classes, music therapy, outdoor excursions, and team-building exercises can encourage social interaction and improve overall well-being.
- Peer Mentoring: Pairing individuals who have successfully completed rehab with those currently undergoing treatment can provide valuable support, guidance, and inspiration. Peer mentoring programs facilitate the sharing of personal experiences, coping strategies, and encouragement, promoting social engagement and motivation for recovery.
- Educational Workshops: Organizing educational workshops on various topics relevant to rehabilitation, such as coping skills, relapse prevention, stress management, and life skills, can encourage social engagement. These workshops allow individuals to learn together, share insights, and build connections with peers who have similar goals.
- Online Support Networks: In today’s digital age, online support networks, forums, and social media groups dedicated to rehabilitation and recovery can provide individuals with a platform for virtual social engagement. These platforms offer a sense of community, allow for information sharing, and provide emotional support even beyond the confines of physical rehab programs.
- Alumni Programs: Establishing alumni programs for individuals who have completed rehab can facilitate ongoing social engagement and support. These programs may include regular meetings, social events, or online platforms where alumni can connect, share experiences, and offer support to those who are still in the recovery process.
- Cultural and Spiritual Activities: Recognizing and respecting the diversity of individuals in rehab, and incorporating cultural and spiritual activities can create a sense of inclusiveness and connection. These activities may include meditation, mindfulness practices, religious services, or cultural celebrations that align with the individual’s beliefs and values.
Promoting social engagement in rehab helps individuals rebuild their social support systems, develop healthy relationships, and feel connected to a larger community, all of which are crucial for sustained recovery and overall well-being.
How to Plan for Old Age Care
6. Make a plan for Adaptation and Assistive Devices for old age rehabilitation
Creating a plan for adaptation and assistive devices in old age rehabilitation involves identifying and implementing tools and modifications to support independence, mobility, and safety. Here’s a general outline to help you create a plan:
- Assess individual needs: Begin by assessing the individual’s specific needs and challenges. This can include evaluating their physical abilities, mobility limitations, and any difficulties they face in performing daily activities. Work with healthcare professionals, such as occupational therapists or physiotherapists, to conduct a thorough assessment.
- Identify areas requiring adaptation: Identify areas or activities where the individual may benefit from adaptations or assistive devices. This can include mobility aids, modifications for home or work environments, and tools to support activities of daily living (ADLs) such as dressing, bathing, or cooking. Pay attention to their specific needs and prioritize adaptations based on the level of impact on their independence.
- Collaborate with healthcare professionals: Consult with healthcare professionals, such as occupational therapists or rehabilitation specialists, to develop a comprehensive adaptation plan. They can provide valuable expertise in recommending suitable assistive devices, modifications, and techniques to address the individual’s specific needs.
- Assistive mobility devices: Assess the need for mobility aids, such as canes, walkers, or wheelchairs, based on the individual’s mobility limitations. Ensure that the devices are properly fitted and provide training on their use. Explore options for portable ramps, grab bars, or stair lifts to facilitate access within the home or community.
- Home modifications: Evaluate the home environment to identify modifications that can enhance safety and accessibility. This may include installing handrails in stairways and bathrooms, improving lighting, removing tripping hazards, or rearranging furniture to create wider pathways. Seek guidance from occupational therapists or home modification specialists to ensure the adaptations meet safety standards.
- Adaptive equipment for ADLs: Introduce adaptive equipment to support the independent performance of ADLs. This can include tools such as teachers, dressing aids, shower chairs, raised toilet seats, or utensils with larger handles. Train the individual on the proper use of these devices to promote self-reliance and reduce the risk of injury.
- Assistive technology: Explore the use of assistive technology to enhance functionality and independence. This can include voice-activated devices, smart home technology, medication reminders, or wearable devices to monitor health or provide emergency assistance. Consider the individual’s comfort level with technology and provide necessary training and support.
- Training and education: Provide training and education on the use of assistive devices and adaptations. This can include demonstration sessions, written instructions, or video tutorials. Ensure that the individual and their caregivers have a clear understanding of how to use and maintain the devices effectively.
- Regular reassessment and adjustments: Regularly reassess the effectiveness of the adaptations and assistive devices. Monitor the individual’s comfort, safety, and level of independence. Make necessary adjustments based on changes in their abilities or needs. Regular follow-up appointments with healthcare professionals can help ensure ongoing support and evaluation.
- Financial resources and support: Explore available financial resources and support to assist with the cost of adaptations and assistive devices. This may include insurance coverage, government programs, grants, or community resources. Investigate eligibility criteria and assist the individual in navigating the application process.
Remember, adaptation and assistive device plans should be personalized to the individual’s specific needs and circumstances. Collaborate with healthcare professionals, occupational therapists, and rehabilitation specialists to obtain personalized recommendations and guidance throughout the rehabilitation process.
6.1 Support Factors in the Adaptation and Assistive Devices for Rehab
During the rehabilitation process, adaptation and assistive devices are often utilized to support individuals in overcoming physical limitations, promoting independence, and enhancing their overall quality of life. Here are some common examples of adaptation and assistive devices used in rehab:
Mobility Aids:

- Canes: Provide stability and support for individuals with balance or walking difficulties.
- Crutches: Assist with weight-bearing and mobility for individuals with lower extremity injuries or impairments.
- Walkers: Offer greater stability and balance support, commonly used by individuals with significant mobility limitations.
- Wheelchairs: Provide mobility for individuals with severe impairments or inability to walk.
Orthoses:
Ankle-Foot Orthoses (AFOs): Assist with foot drop and provide ankle stability.
- Knee Orthoses: Support and stabilize the knee joint for individuals with knee injuries or instability.
- Wrist Splints: Help with wrist stabilization and support during activities for individuals with wrist injuries or conditions like carpal tunnel syndrome.
How to Plan for Old Age Care
Prosthetics:
- Artificial Limbs: Designed to replace missing body parts, such as limbs, with functional prosthetic devices, enabling individuals to regain mobility and perform daily activities.
- Myoelectric Prostheses: Utilize electrical signals generated by the individual’s residual muscles to control the movements of the prosthetic limb.
Adaptive Equipment for Daily Living:
- Researchers and Grabbers: Assist with reaching objects from high or low places for individuals with limited mobility or difficulty bending.
- Dressing Aids: Devices like buttonhooks, zipper pulls, or long-handled shoe horns that aid individuals with limited hand dexterity in dressing independently.
- Adaptive Utensils: Ergonomically designed eating utensils with larger handles or specialized grips for individuals with limited hand function or strength.
- Adaptive Bathroom Equipment: Examples include grab bars, shower chairs, raised toilet seats, and bath transfer benches, which enhance safety and independence in the bathroom for individuals with mobility limitations.
Communication Aids:
- Augmentative and Alternative Communication (AAC) Devices: Assist individuals with speech impairments or communication difficulties by enabling them to communicate using alternative methods such as text-to-speech, picture boards, or eye-tracking devices.
Environmental Control Systems:
- Home Automation Devices: Allow individuals with mobility limitations to control various aspects of their home environment, such as lights, appliances, or temperature, using voice commands or remote controls.
- Voice-activated Assistants: Virtual assistants like Amazon Alexa or Google Assistant can help individuals with limited mobility perform tasks, access information, and control devices using voice commands.
Adaptive Sports and Recreation Equipment:
- Wheelchair Basketball Chairs: Specially designed wheelchairs for playing basketball, offering maneuverability and stability on the court.
- Handcycles: Enable individuals with lower limb impairments to engage in cycling using their upper body strength.
- Adaptive Skis and Snowboards: Modified equipment that allows individuals with physical disabilities to participate in winter sports.
Assistive Technology for Computer Access:
- Voice Recognition Software: Converts spoken words into text, allowing individuals with limited mobility or dexterity to control a computer using voice commands.
- Alternative Keyboards and Mouse Devices: Ergonomically designed keyboards or specialized mouse devices to accommodate individuals with limited hand function or dexterity.
These examples demonstrate the wide range of adaptation and assistive devices available to support individuals during their rehabilitation journey. The selection of specific devices depends on the individual’s unique needs, functional limitations, and goals, and it is important to involve healthcare professionals and therapists who can assess, recommend, and provide proper training for the appropriate use of these devices.
How to Plan for Old Age Care Part – 1 Continue
7. Make a plan of Education and Training for old age rehabilitation
Education and training play a crucial role in old age rehabilitation, promoting cognitive stimulation, skill development, and overall well-being. Here’s a general outline to help you create a plan for education and training:
- Assess individual interests and goals: Begin by assessing the individual’s interests, goals, and learning preferences. Understand their previous educational background and any specific areas of interest they may have. This assessment can be done through conversations, questionnaires, or working with an educational specialist.
- Identify learning opportunities: Identify learning opportunities that align with the individual’s interests and goals. This can include formal education programs, community classes, online courses, workshops, or training sessions specifically designed for older adults. Consider their cognitive abilities, physical capabilities, and access to resources when selecting appropriate options.
- Provide cognitive stimulation: Offer activities that provide cognitive stimulation and mental engagement. This can include puzzles, brain teasers, memory games, or activities that involve problem-solving, critical thinking, and memory recall. Engaging in intellectually stimulating activities helps maintain cognitive function and can contribute to a sense of accomplishment.
- Technology training: Provide training and support in using technology devices and digital platforms. Teach basic computer skills, internet navigation, email usage, and social media engagement. Technology training can enhance digital literacy and enable individuals to connect with others, access online educational resources, and engage in virtual learning experiences.
- Lifelong learning programs: Encourage participation in lifelong learning programs offered by universities, community colleges, or senior centers. These programs often provide a wide range of educational courses and workshops tailored for older adults. Offer courses on topics of interest such as history, literature, art, music, language learning, or practical skills like gardening or cooking.
- Health and wellness education: Provide education and training on topics related to health and wellness. This can include nutrition workshops, exercise classes, stress management techniques, fall prevention programs, or chronic disease management seminars. Enhancing health literacy empowers individuals to make informed decisions about their well-being.
- Personal development workshops: Offer personal development workshops that focus on self-improvement and personal growth. These workshops may cover topics like goal setting, time management, financial planning, communication skills, or creative expression. Personal development programs can contribute to a sense of purpose and fulfillment.
- Intergenerational learning opportunities: Facilitate intergenerational learning experiences where older adults have the opportunity to share their knowledge and skills with younger generations. This can involve mentoring programs, volunteering in schools, or participating in community initiatives that encourage collaboration between different age groups. Intergenerational learning fosters mutual understanding and appreciation.
- Collaborate with local institutions: Establish partnerships with local educational institutions, community centers, or senior organizations to access resources, expertise, and support. These collaborations can provide access to specialized courses, guest speakers, or educational events tailored for older adults. Leverage existing programs and initiatives in the community to enhance the educational opportunities available.
- Evaluate progress and adjust: Regularly evaluate the effectiveness of the education and training plan. Monitor the individual’s engagement, learning outcomes, and overall satisfaction. Seek feedback from the individual and adjust the plan as needed. Continuously explore new opportunities and adapt the educational offerings to meet changing interests and needs.
Remember, education and training plans should be personalized to the individual’s interests, abilities, and learning style. Collaborate with educational specialists, community organizations, and healthcare professionals to obtain tailored recommendations and support throughout the rehabilitation process.
7.1 Support Factors the Education and Training for Rehabilitation:
Education and training are crucial components of rehabilitation programs as they provide individuals with the knowledge, skills, and tools necessary to navigate their recovery journey successfully. Here are some key areas of education and training in rehab:
- Understanding the Condition or Injury: Education about the specific condition or injury being treated is essential for individuals in rehab. This includes learning about the underlying causes, symptoms, and potential complications associated with their condition. Understanding the nature of their condition empowers individuals to make informed decisions and actively participate in their recovery process.
- Treatment Options and Modalities: Rehab programs provide education on various treatment options available for specific conditions. This may include information about medications, therapies (such as physical, occupational, or speech therapy), surgical interventions, assistive devices, and alternative therapies. Individuals learn about the benefits, risks, and expected outcomes of different treatment modalities to make informed choices regarding their care.
- Pain Management and Symptom Control: Education on pain management techniques, symptom control, and strategies for coping with discomfort or other challenging symptoms is crucial in rehab. This includes learning about medication management, relaxation techniques, breathing exercises, and other non-pharmacological interventions to effectively manage pain and symptoms. Read more
- Rehabilitation Techniques and Exercises: Rehab programs provide training on specific rehabilitation techniques and exercises tailored to the individual’s condition and goals. This may include learning therapeutic exercises, stretching routines, range-of-motion activities, and functional training to improve strength, flexibility, balance, and overall physical functioning.
- Assistive Devices and Adaptive Strategies: Education on the use of assistive devices and adaptive strategies is essential for individuals who require support in daily activities. This includes training on the proper use of mobility aids (e.g., canes, crutches, wheelchairs), orthotic devices, adaptive equipment for self-care, and techniques to enhance independence and safety.
- Home Modifications and Safety: Individuals in rehab often require education on home modifications and safety measures to optimize their living environment and prevent future injuries. This includes learning about proper ergonomics, and fall prevention strategies, modifying the home environment for accessibility, and creating a safe and supportive living space.
- Healthy Lifestyle and Self-Care: Education on adopting and maintaining a healthy lifestyle is an integral part of rehab. This may include information on nutrition, exercise, stress management techniques, sleep hygiene, smoking cessation, and substance abuse prevention. Promoting self-care practices empowers individuals to prioritize their physical and emotional well-being.
- Psychosocial Support and Coping Skills: Education and training in psychosocial support and coping skills are vital for individuals in rehab. This includes learning about stress management techniques, emotional regulation strategies, communication skills, problem-solving, assertiveness, and building resilience. These skills enhance emotional well-being, reduce psychological distress, and support long-term recovery.
- Relapse Prevention and Continuing Care: Rehab programs often provide education and training on relapse prevention strategies to minimize the risk of setbacks after completing rehabilitation. This may include identifying triggers, developing effective coping mechanisms, creating a relapse prevention plan, and connecting individuals with support networks and resources for ongoing care.
- Transitioning to Community and Work Life: Education and training on transitioning back to community and work life are important components of rehab. This includes preparing individuals for the challenges they may face in social and vocational settings, providing job training or vocational rehabilitation support, and facilitating community integration and reintegration.
Conclusion:
Education and training in rehab are tailored to the individual’s needs and goals, providing them with the knowledge and skills necessary to manage their condition, optimize their functioning, and promote long-term well-being. Collaborating with a multidisciplinary team of healthcare professionals, therapists, and educators ensures comprehensive and individualized education and training for each individual in rehab.




